Skin Cancer Detection Device
Compiled by Walter Sorochan
Skin cancer is the most common form of human cancer. It is estimated that over 1 million new cases occur annually. The annual rates of all forms of skin cancer are increasing each year, representing a growing public concern. It has also been estimated that nearly half of all Americans who live to age 65 will develop skin cancer at least once.
The most common warning sign of skin cancer is a change in the appearance of the skin, such as a new growth or a sore that will not heal. Types of skin cancer: Basal cell carcinoma is the most common. Melanoma is less common, but more dangerous.
Skin cancer can be prevented and when detected early, can be treated successfully. This article focuses on providing information about prospects of improving early detection.
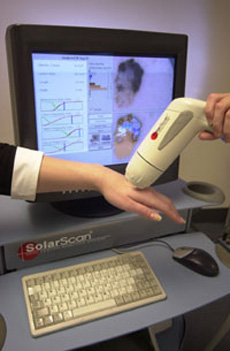
MelaFind is also referred to as "Algorithm Gun.”
 This is a handheld
cancer detection device, which effectively takes a super-fancy 3D photo of skin
lesions, records that data on proprietary memory cards that are
patient-specific, and compares it to their library of skin cancer pics to see
what the likelihood is that this particular lesion is
cancerous or worthy of
aggressive treatment.
This is a handheld
cancer detection device, which effectively takes a super-fancy 3D photo of skin
lesions, records that data on proprietary memory cards that are
patient-specific, and compares it to their library of skin cancer pics to see
what the likelihood is that this particular lesion is
cancerous or worthy of
aggressive treatment.
Technology used:
C-VS Tech or Computer
Vision Systems Technology.
Computer vision
is the science and technology of machines that see.
Computer vision is the branch of
artificial intelligence that focuses on providing computers with the functions
typical of human vision. To date, computer vision has produced important
applications in fields such as industrial automation, robotics, biomedicine, and
satellite observation of Earth. In the field of industrial automation alone, its
applications include guidance for robots to correctly pick up and place
manufactured parts, nondestructive quality and integrity inspection, and on-line
measurements.

Applications include: human recognition of fingerprints, eyes, faces, voices, DNA, video surveillance, recognize of behavior, detection of body disorders like skin cancer, airport check for weapons, poultry industry, military applications & so on.
FDA: used a guideline in 2009 called "PMA/510(k) Expedited Review," to essentially speed up the review process for this new device for diagnosing a life-threatening disease on assumption that it "represents a breakthrough technology that provides a clinically meaningful advantage of existing technology."
To evaluate a
biomedical-screening device like the "Algorithm Gun", you must answer two
questions:
1) Does the device catch the
disease (the sensitivity)?
2) Does it also tell you who's disease-free (the specificity)?
In a preliminary study of
352 lesions, this company’s device correctly identified all 28 cancers. And in
all tests so far, the company’s device has correctly diagnosed cancer in 98% of
the cases, compared to the 60% to 70% rate doctors are able to identify the
disease using the ABCDE method.
 Competitors:
Competitors:
Similar product (SolarScan) has been around in
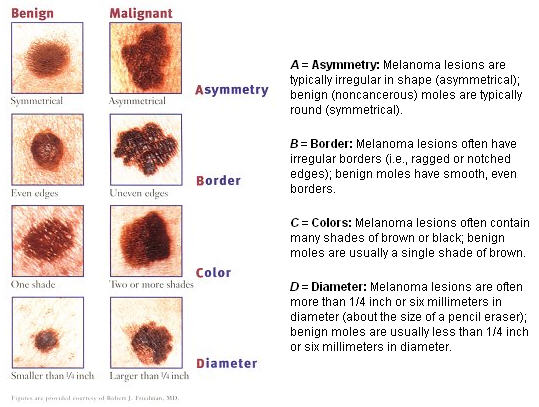
ABCD's of melanoma:
The simple ABCD approach is a useful guide to help you identify moles you should show your doctor:
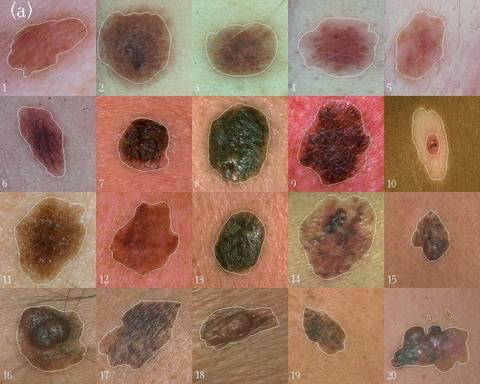
Stages of melanoma:
There are four stages of
melanoma that classify the severity of this skin cancer.
Each stage
pertains to the thickness and the amount that the melanoma has spread.
When the stage of melanoma has been diagnosed, it is then possible for the
doctors to determine the best type of treatment. In this article, we will
discuss what the different stages of melanoma signify. We will describe each of
the four stages in further detail. Hopefully, after reading this article you
will have a greater knowledge of the skin cancer disease known as melanoma and
the four degrees associated with it.
Stage 1 of melanoma is thin and the
epidermis usually appears scraped. This stage of skin cancer is subdivided into
two other categories. These additional categories describe the thickness of the
tumor. Stage 1a is less than 1.0 mm and has no ulceration. Stage 1b is less than
1.0 mm but has ulceration. It is also considered to be in stage 1b if it is 1.01
- 2.0 mm even if it does not involve ulceration. In this stage and stage 2 the
melanoma has not yet spread to the lymph nodes.
Stage 2 is also subdivided into three
more categories that signify the thickness and the existence or non-existence of
ulceration. The tumor in stage 2a is 1.01 - 2.0 mm with ulceration or 2.01 - 4.0
mm without ulceration. Stage 3b has a tumor thickness of 2.01 with ulceration or
a thickness of more than 4.0 without ulceration.
When this type of skin cancer advances to
stage 3 a significant change occurs. At this stage, the melanoma tumor has
spread to the lymph nodes. This is a much more serious stage of the disease
because when healthy, the lymph nodes fight disease, cancer and some other
infections.
Patients with stage 3 of this cancer
have melanoma that has spread into lymph nodes near the primary tumor. This
stage also involves in-transit metastasis that has skin or connective tissue
that is more than 2 centimeters from the original tumor. However, at this point
it has not spread past the regional lymph nodes.
In stage 4, the melanoma has spread
to lymph nodes that are a distance from the original tumor or to internal
organs. These organs are most often the lung, liver, brain, bone and then the
gastrointestinal tract.
When diagnosed with skin cancer, it is important to consult with your doctor
concerning the degree or stage of melanoma that you may have. A variety of
diagnostic techniques will likely be used to determine the stage of your skin
cancer. Most stage 1 and stage 2 melanomas should not cause too much worry
because they can most often be cured through surgery. There is little need to
worry about getting later stages of melanoma just because you once suffered
through the early stages.
Different doctors may use different
systems or scales to classify the stages of melanoma. The most commonly used
are the TNM
staging system and the Breslow scale. The most important things to
remember are that melanomas with 0.76 mm or lower thickness are low risk, 0.76 -
1.5 mm involve medium risk and when the melanoma is more than 1.5 mm in
thickness you are at a much higher risk. When you are diagnosed with melanoma it
is important that you understand exactly what stages your doctor may be
referring to and what treatments are available to you.
Web: http://seekingalpha.com/article/154027-fda-calendar-updates-viropharma-electro-optical-sciences-wyeth-progenics